Mosby’s Pocket Guide to Fetal Monitoring provides a comprehensive‚ evidence-based resource for healthcare professionals. Authored by experts‚ it offers practical insights into fetal heart rate interpretation and monitoring techniques‚ ensuring accurate and informed clinical decisions. Its compact design makes it an essential tool for daily use in obstetric care settings.
History of Fetal Monitoring
Fetal monitoring has evolved significantly since its inception‚ becoming a cornerstone in modern obstetric care. The origins trace back to early attempts to auscultate fetal heart sounds‚ with advancements in electronic monitoring emerging in the mid-20th century. Key milestones include the development of cardiotocography and fetal scalp pH sampling‚ which laid the groundwork for contemporary practices. Mosby’s Pocket Guide highlights how fetal monitoring transitioned from a specialized tool to a widely adopted standard in both high-risk and low-risk pregnancies‚ revolutionizing prenatal and intrapartum care. This historical context underscores its critical role in improving maternal and fetal outcomes.

Physiologic Basis of Fetal Heart Rate Monitoring
Fetal heart rate monitoring is rooted in understanding fetal physiology and the relationship between heart rate patterns and fetal well-being. The guide explains how fetal heart rate reflects placental function‚ fetal oxygenation‚ and the autonomic nervous system’s role in regulating heart rate variability. This foundation is crucial for interpreting patterns and assessing fetal status accurately during pregnancy and labor‚ enabling timely interventions to ensure optimal outcomes. The text emphasizes the importance of understanding these physiologic principles to apply monitoring effectively in clinical practice.
3.1. Physiology of Fetal Heart Rate
The fetal heart rate (FHR) is regulated by the autonomic nervous system‚ reflecting fetal well-being and oxygenation. Normal FHR ranges from 110 to 160 beats per minute‚ influenced by gestational age‚ sleep cycles‚ and maternal factors. Accelerations in FHR during labor often indicate fetal movement and adequate oxygen supply‚ while decelerations may signal stress. Understanding these physiological principles is essential for accurate interpretation of FHR patterns‚ enabling healthcare providers to assess fetal status and make informed clinical decisions. This section provides a detailed overview of the mechanisms controlling FHR and their implications for fetal monitoring.
3.2. Relationship Between Fetal Heart Rate Patterns and Neonatal Outcomes
Fetal heart rate (FHR) patterns are critical indicators of fetal well-being‚ directly correlating with neonatal outcomes. Normal patterns‚ such as accelerations during fetal movement‚ often predict healthy outcomes‚ while abnormal patterns‚ like persistent decelerations‚ may indicate fetal distress. Research shows that accurate interpretation of FHR tracings can help identify at-risk infants‚ enabling timely interventions. This section emphasizes the importance of understanding FHR patterns to improve neonatal health and reduce complications. By linking FHR monitoring to clinical outcomes‚ healthcare providers can make informed decisions‚ enhancing maternal and fetal care.
Methods and Instrumentation in Fetal Monitoring
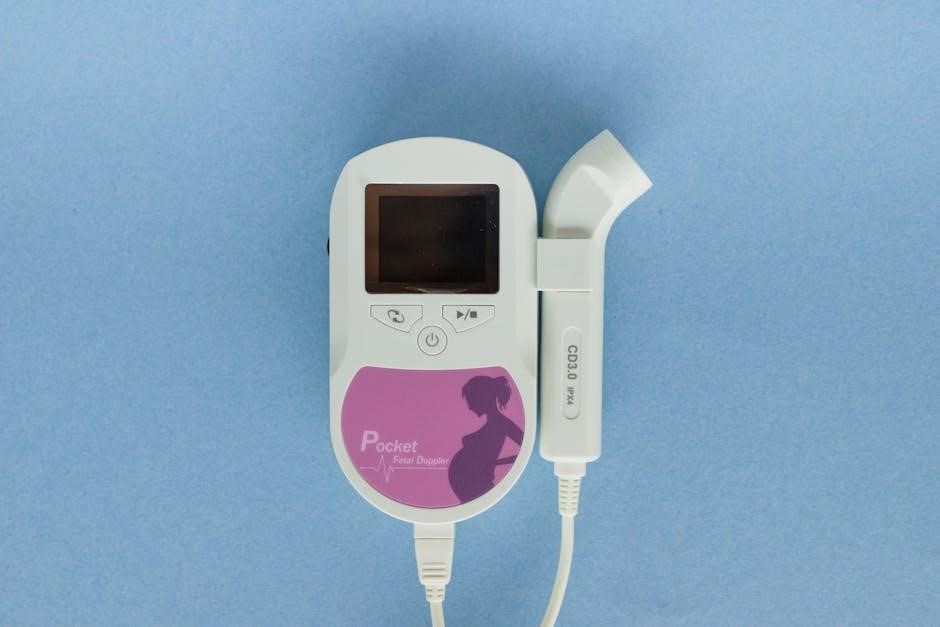
Fetal monitoring employs both continuous and intermittent methods‚ utilizing advanced technologies like electronic fetal monitoring (EFM) and Doppler devices. These tools provide real-time data on fetal heart rates‚ enabling precise assessments and informed clinical decisions during pregnancy‚ labor‚ and postpartum care.
4.1. Types of Fetal Monitoring: Continuous vs. Intermittent
Fetal monitoring is categorized into continuous and intermittent methods. Continuous monitoring‚ often used in high-risk pregnancies‚ provides real-time data on fetal heart rate (FHR) and uterine contractions using devices like cardiotocography. Intermittent monitoring‚ suitable for low-risk pregnancies‚ involves periodic checks of FHR using handheld Doppler or auscultation. Continuous monitoring offers immediate insights into fetal well-being during labor‚ while intermittent monitoring allows for greater patient mobility and is typically used in antepartum settings. Understanding these methods is crucial for tailoring care to individual needs‚ ensuring accurate assessments‚ and supporting clinical decision-making.
4.2. Technology and Equipment Used in Fetal Monitoring
Fetal monitoring employs advanced technologies to assess fetal well-being. Cardiotocography (CTG) is a primary tool‚ combining fetal heart rate (FHR) and uterine contraction monitoring. Fetal scalp electrodes provide precise FHR data‚ while external Doppler devices offer non-invasive alternatives. Handheld Dopplers and fetal stethoscopes are used for intermittent monitoring. Modern systems integrate maternal vital signs and fetal data‚ enhancing comprehensive care. These technologies ensure accurate assessments‚ aiding clinicians in timely decision-making and improving outcomes. The guide details how to select and utilize these tools effectively‚ ensuring optimal fetal monitoring in diverse clinical scenarios.
Standardized Terminology and Pattern Recognition
Mosby’s guide provides standardized terminology and methods for interpreting fetal heart rate patterns‚ ensuring consistency in clinical decision-making and communication among healthcare professionals.
5.1. Key Terms and Definitions
Mosby’s guide defines essential terms for fetal monitoring‚ such as baseline fetal heart rate‚ variability‚ accelerations‚ and decelerations. These definitions provide a clear framework for interpreting patterns accurately‚ ensuring consistency in clinical communication and documentation. The guide also clarifies terms like “early‚” “late‚” and “variable” decelerations‚ as well as “sinusoidal” patterns‚ to enhance understanding and application in practice. Standardized language helps healthcare professionals identify and respond to fetal status changes effectively‚ promoting precise and reliable care during pregnancy‚ labor‚ and delivery. This section serves as a foundational reference for clinicians to master the vocabulary of fetal heart rate monitoring.
5.2. Interpreting Fetal Heart Rate Patterns
Mosby’s guide provides a structured approach to interpreting fetal heart rate (FHR) patterns‚ emphasizing the importance of acceleration and deceleration analysis. It highlights normal versus concerning patterns‚ such as late decelerations‚ which may indicate fetal distress. The guide emphasizes the role of baseline rate variability in assessing fetal well-being. Clear examples and criteria help clinicians distinguish between reassuring and non-reassuring tracings. This section also discusses the significance of sinusoidal patterns and their clinical implications. By focusing on evidence-based interpretation‚ the guide enables healthcare providers to make informed decisions‚ ensuring accurate and timely interventions for improved neonatal outcomes.
Evidence-Based and Collaborative Approach
Mosby’s guide emphasizes evidence-based practices and multidisciplinary collaboration‚ combining expertise from nurses‚ midwives‚ and physicians to optimize fetal monitoring and maternal care‚ ensuring comprehensive and unified patient management.
6.1. Multidisciplinary Collaboration in Fetal Monitoring
Mosby’s Pocket Guide emphasizes the importance of multidisciplinary collaboration in fetal monitoring‚ involving nurses‚ midwives‚ and physicians. This teamwork enhances communication‚ ensures accurate interpretations of fetal heart rate patterns‚ and improves clinical decision-making. The guide highlights how collaboration between healthcare professionals leads to better patient safety and outcomes. By integrating expertise from various disciplines‚ it provides a unified approach to monitoring‚ ensuring comprehensive care for mothers and fetuses. This collaborative framework is essential for addressing complex scenarios and achieving optimal results in both antepartum and intrapartum settings.

Clinical Applications of Fetal Monitoring
Mosby’s guide covers fetal monitoring across antepartum‚ intrapartum‚ and postpartum periods‚ ensuring continuous assessment and timely interventions‚ supporting clinical decisions and improving neonatal outcomes.
7.1. Antepartum Fetal Monitoring
Antepartum fetal monitoring assesses fetal well-being before labor‚ ensuring early detection of potential complications. Methods include non-stress tests and biophysical profiles‚ providing insights into fetal health and guiding clinical decisions.
7.2. Intrapartum Fetal Monitoring
Intrapartum fetal monitoring occurs during labor to assess fetal well-being continuously. It involves tracking fetal heart rate patterns and uterine contractions using electronic devices. This method helps identify potential fetal distress or complications‚ guiding timely interventions such as oxygen administration or expedited delivery. The guide emphasizes accurate interpretation of heart rate tracings to ensure optimal outcomes‚ supporting healthcare providers in making informed decisions during labor. Its evidence-based approach ensures safe and effective monitoring practices‚ aligning with current clinical standards and enhancing patient care during this critical phase.
7.3. Postpartum Fetal Monitoring
Postpartum fetal monitoring focuses on assessing the newborn’s transition from fetal to neonatal life. It involves evaluating heart rate patterns‚ vital signs‚ and overall adaptation post-delivery. This period is critical for identifying potential complications early‚ ensuring a smooth transition for the baby. The guide provides evidence-based recommendations for postpartum care‚ emphasizing the importance of continuous observation and collaboration between healthcare providers. It also highlights the role of monitoring in detecting abnormalities and ensuring the newborn’s safety during this vulnerable phase. The approach aligns with modern clinical standards‚ offering a comprehensive framework for postpartum fetal care and transition to neonatal management.
Patient Safety and Quality Improvement
Mosby’s guide emphasizes evidence-based practices to enhance patient safety‚ minimize risks‚ and improve fetal monitoring outcomes‚ addressing legal and ethical considerations in perinatal care.
8.1. Enhancing Patient Safety Through Monitoring
Mosby’s guide highlights the critical role of fetal monitoring in enhancing patient safety by enabling early detection of potential complications. Continuous and accurate surveillance allows healthcare providers to identify abnormalities promptly‚ facilitating timely interventions. This approach reduces the risk of adverse neonatal outcomes and improves overall maternal-fetal well-being. By adhering to evidence-based protocols‚ clinicians can ensure safer care practices. The guide also emphasizes the importance of interdisciplinary collaboration and clear communication in maintaining high standards of safety. Regular monitoring further supports quality improvement initiatives‚ ensuring that care aligns with current best practices and legal-ethical standards in perinatal medicine.
8.2. Legal Implications of Fetal Monitoring
Mosby’s guide addresses the legal implications of fetal monitoring‚ emphasizing the importance of accurate documentation and adherence to established standards of care. Proper use of monitoring tools can serve as a legal defense‚ demonstrating that care was provided in accordance with professional guidelines. Conversely‚ errors in interpretation or documentation may lead to liability concerns. The guide provides clear recommendations for minimizing legal risks‚ ensuring that healthcare providers understand their responsibilities and the potential consequences of mismanagement. It also highlights the role of monitoring in supporting ethical practices and maintaining patient trust. Legal considerations are integrated throughout the text to promote compliance and risk reduction.
Authors’ Expertise and Contributions
9.1. Integration into Educational Programs
Mosby’s Pocket Guide to Fetal Monitoring is widely integrated into educational programs for healthcare professionals. Its clear‚ evidence-based content supports training in fetal heart rate interpretation and monitoring. The guide’s collaborative approach‚ involving nurse-midwives‚ perinatologists‚ and nurses‚ ensures comprehensive learning. It emphasizes standardized terminology and pattern recognition‚ aligning with curriculum goals. The pocket-sized format makes it a practical resource for students and clinicians alike‚ enhancing both theoretical knowledge and clinical skills. By incorporating real-world examples and evidence-based recommendations‚ the guide serves as an invaluable tool for fostering competency in fetal monitoring across diverse educational settings.
Guide Format and Usability
Mosby’s Pocket Guide to Fetal Monitoring features a compact‚ easy-to-carry design‚ making it highly practical for clinical use. Its clear layout ensures quick access to essential information‚ enhancing usability for healthcare professionals in fast-paced environments.
10.1. Pocket-Sized Format for Practical Use
Mosby’s Pocket Guide to Fetal Monitoring is designed as a portable‚ lightweight resource‚ perfect for clinical settings. Its compact size allows easy carrying in a lab coat or bag‚ ensuring accessibility during patient care. The durable design withstands frequent use‚ and its spiral binding enables quick page flips for efficient reference. Water-resistant pages protect the content‚ and clear typography enhances readability. This format caters to busy healthcare professionals‚ providing essential fetal monitoring insights without compromising convenience. Its practical design aligns with the demands of dynamic obstetric environments‚ making it an indispensable tool for daily practice.

Evidence-Based Practice and Recommendations
Mosby’s Pocket Guide to Fetal Monitoring emphasizes evidence-based practice‚ providing clear‚ research-supported recommendations for interpreting fetal heart rate patterns. It integrates the latest clinical findings and guidelines‚ ensuring healthcare providers can make informed decisions. The guide highlights the importance of a collaborative approach‚ combining medical and nursing perspectives to enhance patient outcomes. By focusing on peer-reviewed literature and established protocols‚ it offers a reliable framework for fetal monitoring. This section underscores the importance of staying updated with current research and best practices‚ ensuring safe and effective care for mothers and newborns.

Training and Education in Fetal Monitoring
Mosby’s Pocket Guide to Fetal Monitoring serves as a valuable educational tool‚ offering practical insights and training for healthcare professionals in fetal heart rate interpretation and monitoring techniques.
12;1. Integration into Educational Programs
Mosby’s Pocket Guide to Fetal Monitoring is seamlessly integrated into educational programs‚ providing students and healthcare professionals with a concise‚ evidence-based resource. The guide supports curriculum development by offering practical‚ real-world examples of fetal heart rate interpretation and monitoring techniques. Its peer-reviewed discussions and comprehensive approach make it an invaluable tool for training programs in nursing‚ midwifery‚ and obstetrics. The guide’s clear structure and portability enhance its effectiveness in both classroom and clinical settings‚ ensuring learners gain the skills and knowledge needed for accurate fetal monitoring and informed decision-making in maternity care.

Future Directions in Fetal Monitoring
Future advancements in fetal monitoring include improved sensor technologies‚ AI-driven pattern analysis‚ and enhanced portability. These innovations aim to refine accuracy‚ accessibility‚ and clinical decision-making in obstetric care.
13.1. Emerging Technologies and Trends
Emerging technologies in fetal monitoring include advanced sensors‚ AI-driven systems‚ and wearable devices. These innovations enhance accuracy and accessibility‚ enabling real-time‚ continuous monitoring. AI algorithms improve pattern recognition‚ reducing interpretation errors. Wireless and portable devices allow for remote monitoring‚ benefiting high-risk pregnancies. Additionally‚ advancements in data integration with electronic health records streamline care coordination. These technologies aim to enhance patient safety‚ improve outcomes‚ and provide more personalized obstetric care. As research progresses‚ fetal monitoring is expected to become more precise‚ non-invasive‚ and widely accessible‚ revolutionizing prenatal and intrapartum care globally.
Mosby’s Pocket Guide to Fetal Monitoring is an indispensable resource for healthcare professionals‚ offering a comprehensive and evidence-based approach to fetal heart rate monitoring. Authored by a multidisciplinary team of experts‚ it bridges theory and practice‚ providing clear guidance for clinical decision-making. The guide emphasizes patient safety‚ collaboration‚ and the integration of emerging technologies. Its practical format and usability make it a valuable tool for both seasoned practitioners and students. By staying current with advancements in fetal monitoring‚ this guide ensures improved outcomes for mothers and newborns‚ solidifying its role as a cornerstone in modern obstetric care.

